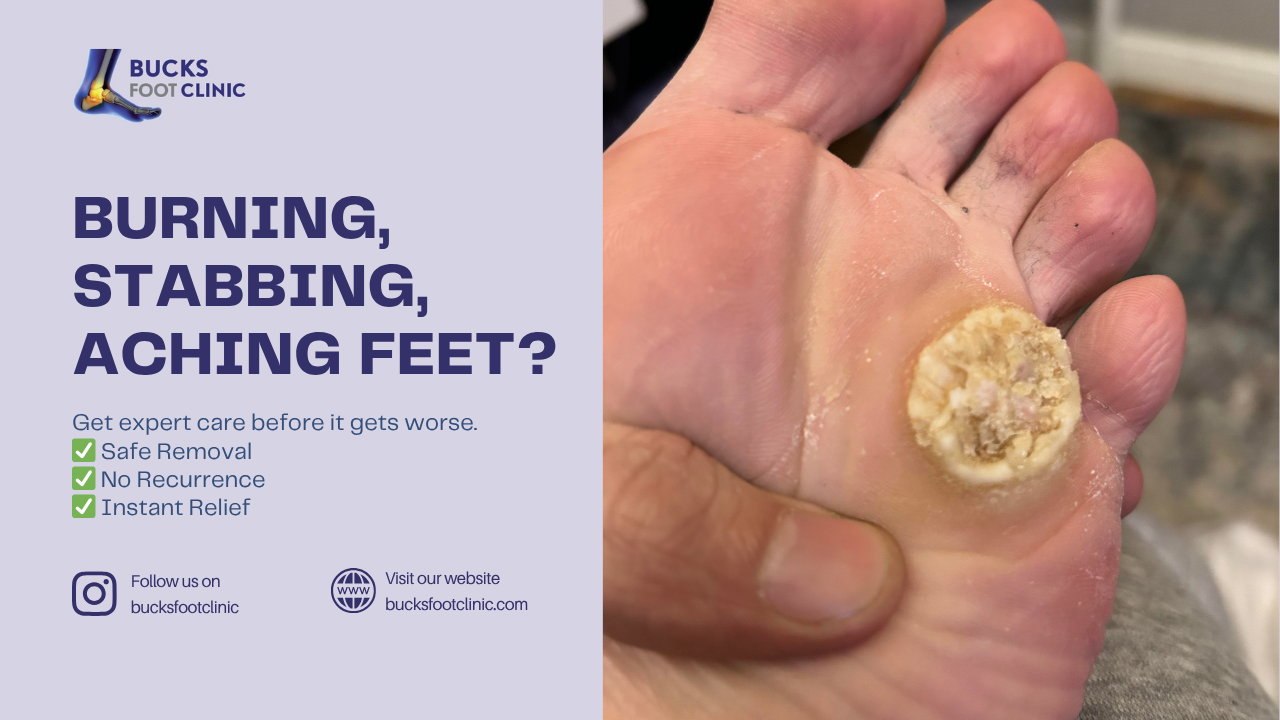
Corns might seem like a minor issue, but their impact on daily life can be anything but. These hardened patches of skin, caused by repeated pressure or friction, can turn each step into a painful ordeal. While DIY remedies promise quick fixes, they often lead to more harm than good. This article explores why corns hurt, why professional care is your best bet, and how to reclaim pain-free feet with expert podiatric treatment.
Why Do Corns Hurt So Much?
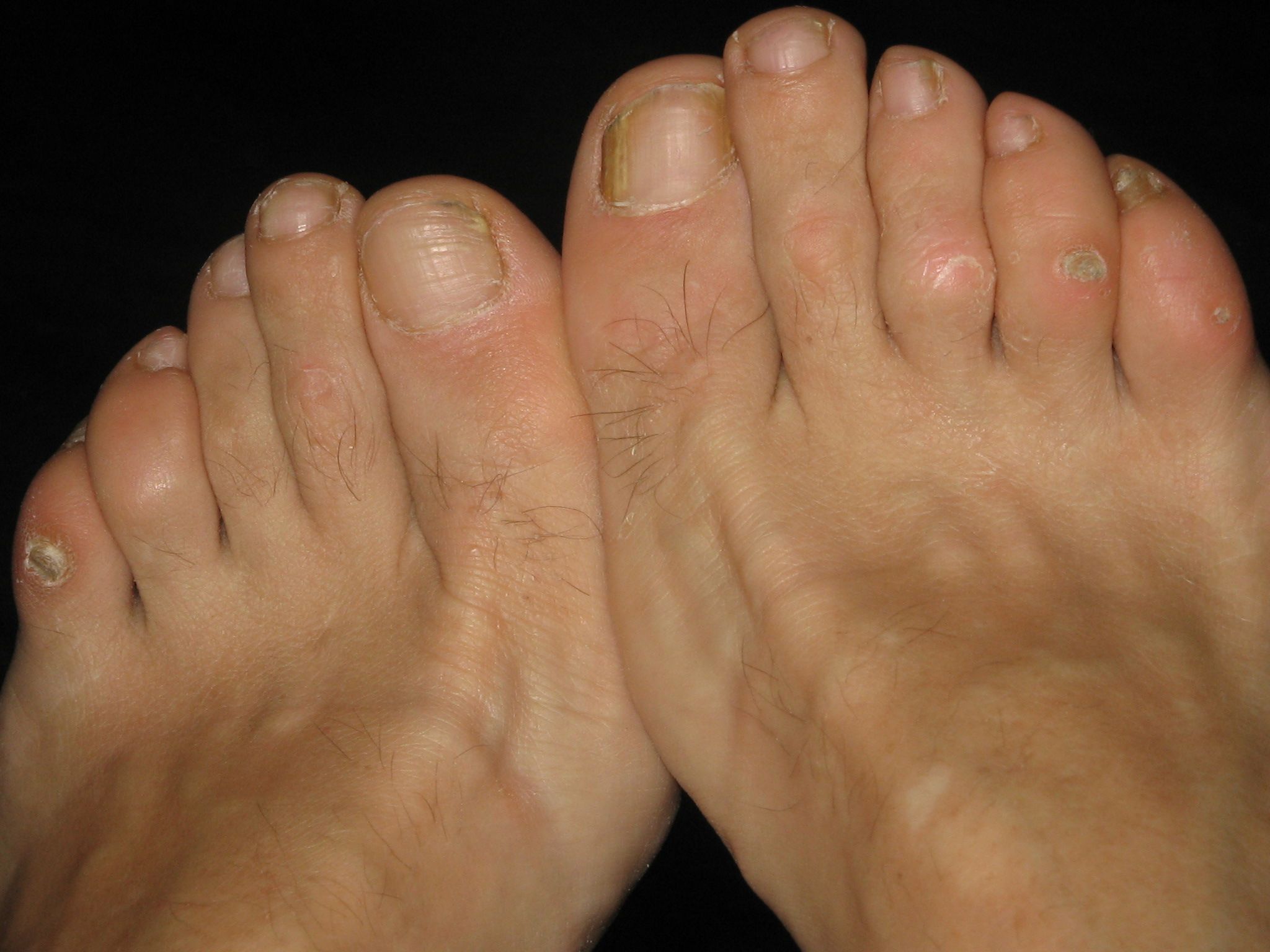
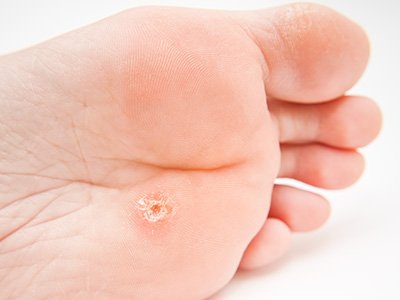
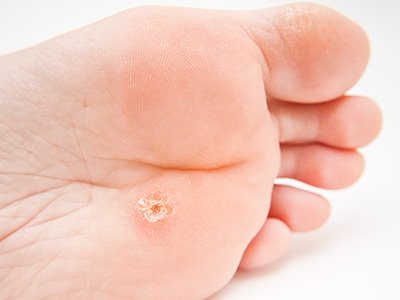
Corns develop in areas of the feet that bear repeated pressure, such as the tops of toes or the balls of your feet. Over time, this pressure causes the thickened skin to press into deeper tissues, irritating nerves and triggering pain. Here’s what makes corns so bothersome:
- Burning Pain: Prolonged irritation can make the affected area feel like it’s on fire.
- Sharp, Stabbing Pain: Corns pressing on nerves create intense, localized pain with every step.
- Persistent Ache: Even at rest, corns can cause a dull, throbbing discomfort.
- Extreme Sensitivity: Light touches, such as from socks or shoes, can feel unbearable.
For those with conditions like diabetes or poor circulation, corns pose even greater risks, such as infections and ulcers, making professional care essential.
DIY Corn Treatments: Why They Often Fail
While it’s tempting to try over-the-counter solutions or home remedies, many DIY approaches can worsen the problem. Here’s why:
1. Pumice Stones and Over-Scrubbing
Using a pumice stone can be helpful, but overdoing it removes too much skin, leading to bleeding, sensitivity, and infection risks.
2. Corn Pads with Chemicals
These often contain salicylic acid, which softens the corn but also damages surrounding healthy skin, causing irritation or burns.
3. Sharp Tools
Attempting to cut or scrape a corn at home is risky. Deep cuts can lead to wounds, infections, and long-term scarring.
4. Ignoring the Root Cause
DIY treatments often fail to address why the corn formed in the first place, such as poor footwear or gait issues. Without fixing the underlying problem, the corn is likely to return.
5. Infection Risks
Small nicks or cuts caused by home treatments create perfect entry points for bacteria, leading to swelling, redness, and pus formation.
Home Treatments That Help (and What to Avoid)
While professional care is the gold standard, there are safe home treatments that can offer temporary relief:
Do’s:
- Warm Soaks: Soak your feet in warm water with Epsom salts to soften corns and reduce discomfort.
- Moisturise Regularly: Apply a foot cream to keep the skin around your corn hydrated and less prone to cracking.
- Cushioning Pads: Use non-medicated pads to protect the corn from pressure.
- Wear Comfortable Shoes: Opt for footwear with ample room for your toes and cushioned soles.
Don’ts:
- Avoid Aggressive Scrubbing: Gentle use of a pumice stone is fine, but avoid over-scrubbing.
- Say No to Corn Pads with Chemicals: These can harm healthy skin around the corn.
- Don’t Pick or Cut: Leave the sharp tools to the professionals to avoid infections and complications.
Why Professional Podiatric Care is a Game-Changer
When it comes to lasting relief, podiatrists provide treatments that are safer, more effective, and tailored to your needs. Here’s what sets professional care apart:
1. Accurate Diagnosis
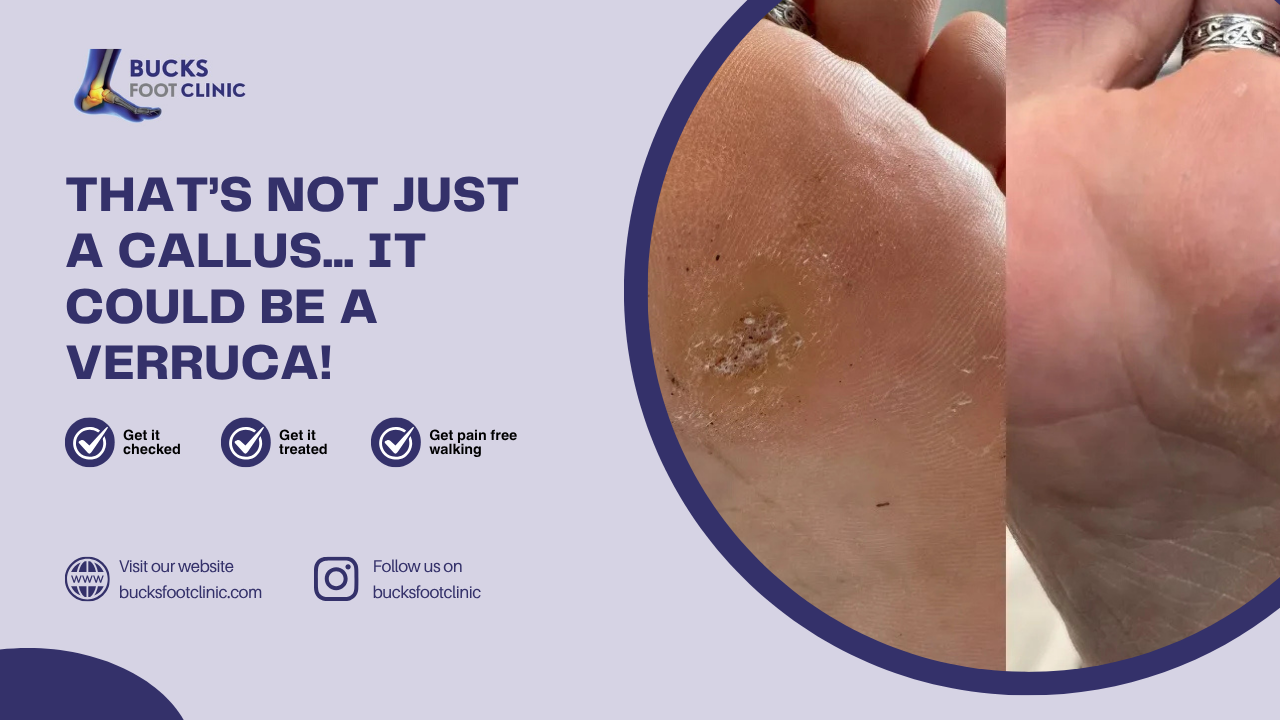
Not all thickened skin is a corn. A podiatrist ensures an accurate diagnosis, ruling out similar conditions like calluses or warts.
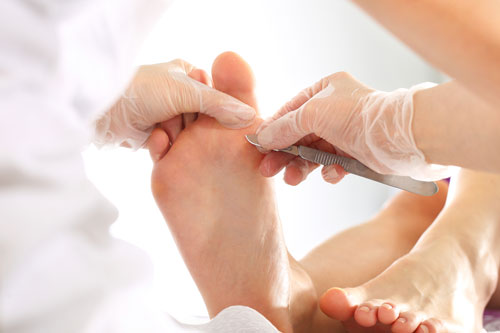
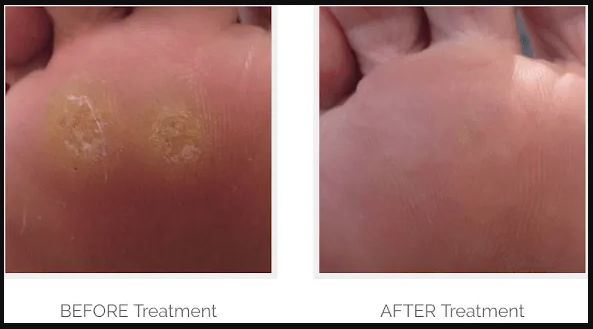
2. Pain-Free Corn Removal
Using sterile tools and precise techniques, podiatrists can safely remove corns without damaging surrounding tissue, offering immediate relief.
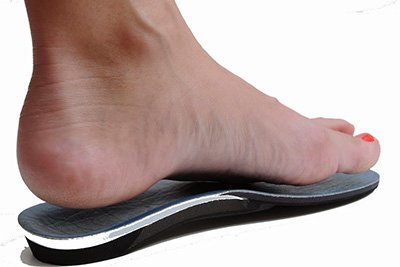
3. Addressing the Root Cause
From custom orthotics to gait analysis, podiatrists identify and correct the underlying issues causing your corns, ensuring they don’t return.
4. Infection Prevention
If a corn is already infected, podiatrists use advanced treatments to clean and heal the area safely.
5. Comprehensive Skin Care
Beyond corn removal, podiatrists provide guidance on maintaining healthy, resilient skin through proper moisturising and protective measures.
The Hidden Costs of Ignoring Corns
Leaving corns untreated can have long-term consequences, including:
- Altered Walking Patterns: Avoiding corn pain can strain your knees, hips, and back, leading to joint and muscle issues.
- Recurring Infections: Persistent corns can become infected, requiring more intensive treatments.
- Chronic Sensitivity: Neglecting corns can leave the skin permanently sensitive and prone to further issues.
When to See a Podiatrist
Wondering if it’s time to seek professional help? Book an appointment if:
- Pain persists despite basic care.
- Swelling, redness, or signs of infection appear.
- Corns keep coming back, even after treatment.
- Foot pain affects your walking or daily activities.
- You have diabetes or circulation issues, making your feet more vulnerable to complications.
Your Feet Deserve Expert Care
At Bucks Foot Clinic, we’re dedicated to helping you walk pain-free. Our podiatrists offer tailored treatments to remove corns, address their causes, and prevent recurrence. Serving Amersham, Chesham, and Little Chalfont, we combine expertise with a patient-focused approach to ensure your feet stay healthy and comfortable.
Why Wait? Get Expert Care Today!
Corns may start as a minor inconvenience, but the pain and complications they cause can quickly escalate. While home remedies may seem convenient, they often lead to further damage and recurring issues. Professional podiatric care is the safest and most effective way to treat corns, alleviate pain, and prevent future problems. At Bucks Foot Clinic, our expert podiatrists are committed to helping you walk comfortably and confidently. Don’t let corns hold you back
Book your appointment today and step into a pain-free future!
FAQ
What causes corns on feet?
Corns develop due to repeated pressure or friction, often from poorly fitting shoes or abnormal walking patterns.
How can I prevent corns?
Wear well-fitted shoes, use cushioned insoles, and avoid prolonged pressure on specific areas of your feet.
Are over-the-counter corn pads effective?
They may provide temporary relief but can irritate healthy skin and fail to address the root cause.
What is the best treatment for corns?
Professional removal by a podiatrist, combined with advice on prevention, is the most effective solution
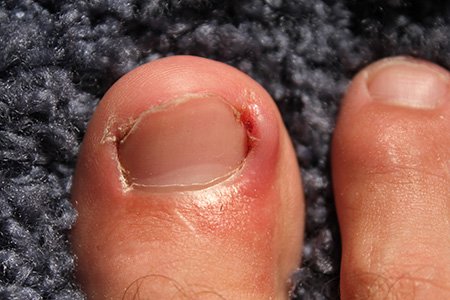
Can toenail pain indicate a serious condition?
Persistent pain may signal infections or underlying issues that require professional care.
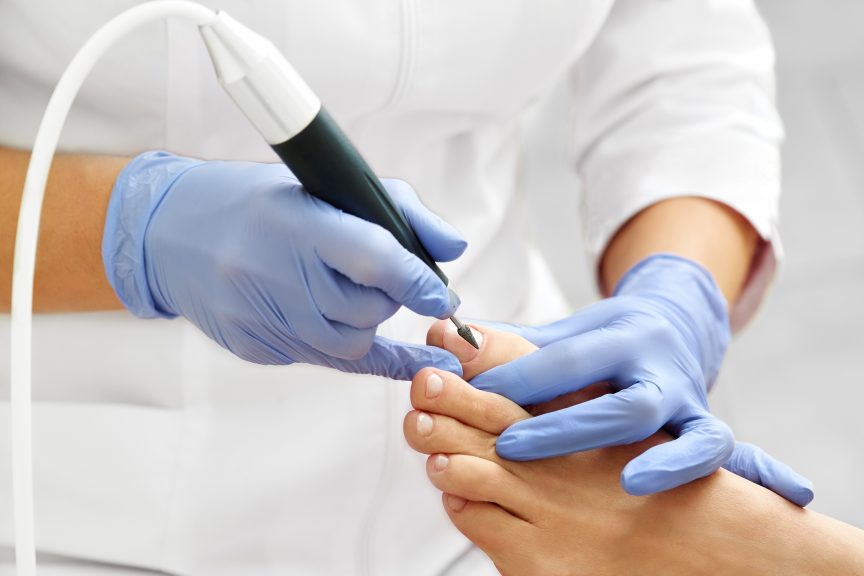
How does Bucks Foot Clinic treat toenail pain?
We offer a range of treatments, including safe nail trimming, antifungal care, and minimally invasive procedures like PNA.
How do I prevent toenail infections?
Maintain good foot hygiene, wear breathable socks, and trim nails correctly.
Is toenail pain common?
Yes, it’s a frequent issue that can often be resolved with proper care.
Are treatments at Bucks Foot Clinic effective?
Yes, our podiatrists use advanced techniques to ensure long-lasting relief.
How do I book an appointment at Bucks Foot Clinic?
Visit our website or call us directly to schedule a consultation with our expert podiatrists.








































Recent Comments