Hello, I’m Dr. Leena Lakhani, a podiatrist at Bucksfoot Clinic. Today, we’re diving into the world of verrucas. If you’ve ever wondered what these pesky skin lesions are, how they develop, and who can help you get rid of them, you’ve come to the right place.
In this blog, we’ll explore the ins and outs of verrucas, including their causes, formation, appearance, spreading, and most importantly, how a podiatrist can professionally treat them, ensuring you can confidently put your best foot forward.
What Are Verrucas?
Verrucas, also known as plantar warts, are small, rough growths on the soles of the feet. They are caused by the human papillomavirus (HPV) and are highly contagious. Although verrucas are typically benign and don’t pose a significant health risk, they can be uncomfortable and unsightly.
What Causes Verrucas?
Verrucas, those small but bothersome growths on the soles of your feet, are primarily the result of infection with specific strains of the Human Papillomavirus (HPV). The most prevalent culprits in the verruca world are HPV types 1, 2, and 4.
Now, let’s delve a bit deeper into how this common virus takes root on your feet:
- HPV in Warm, Moist Environments: The Human Papillomavirus thrives in warm, moist environments. This preference makes the feet an ideal location for their development. When you walk barefoot in public places such as swimming pools, locker rooms, or communal showers, you expose your feet to these virus-containing environments.
- Gateway Through Compromised Skin: In its quest to establish itself, HPV requires an entry point, and it often finds one through minor breaches in the skin’s protective barrier. These can be as innocuous as a tiny cut, a scratch, or even skin softened by prolonged exposure to moisture. It’s at these weakened points that the virus gains a foothold.
Once the HPV enters through these microscopic openings, it starts to infect the outer layer of your skin, leading to the development of verrucas. The virus triggers an increase in cell growth, causing the skin cells to multiply more rapidly. This acceleration in cell division, combined with the body’s natural response to HPV, results in the characteristic appearance of a verruca.
How Do They Form?
Verrucas form when the HPV virus enters the body through minor breaks in the skin, such as those you might incur while walking barefoot in communal areas like swimming pools, locker rooms, or public showers. The virus then infects the outer layer of skin, leading to the development of verrucas.
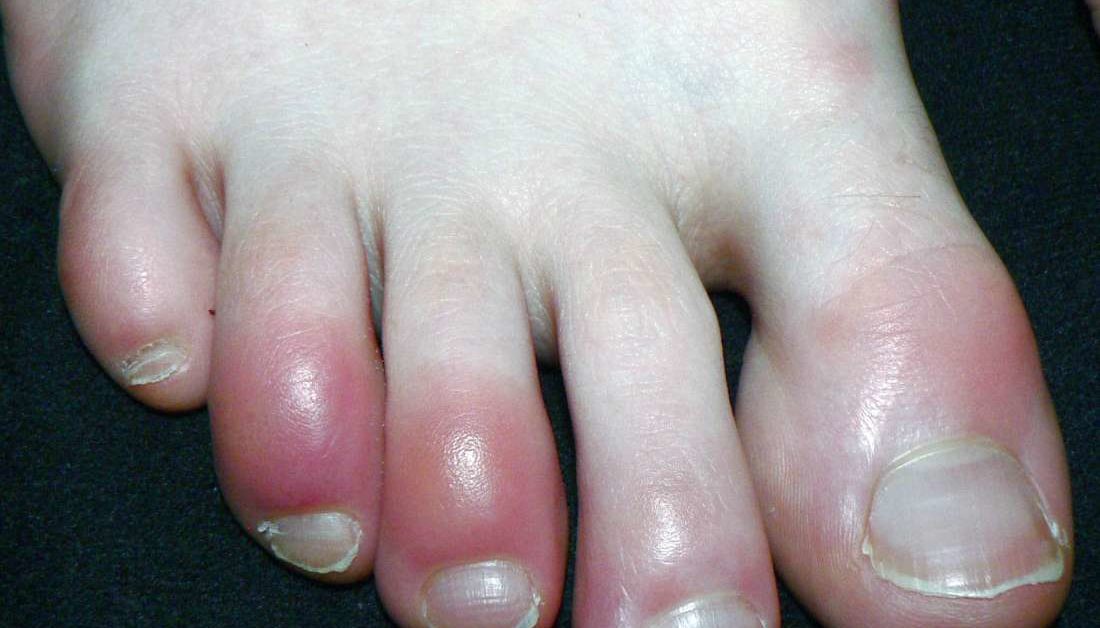
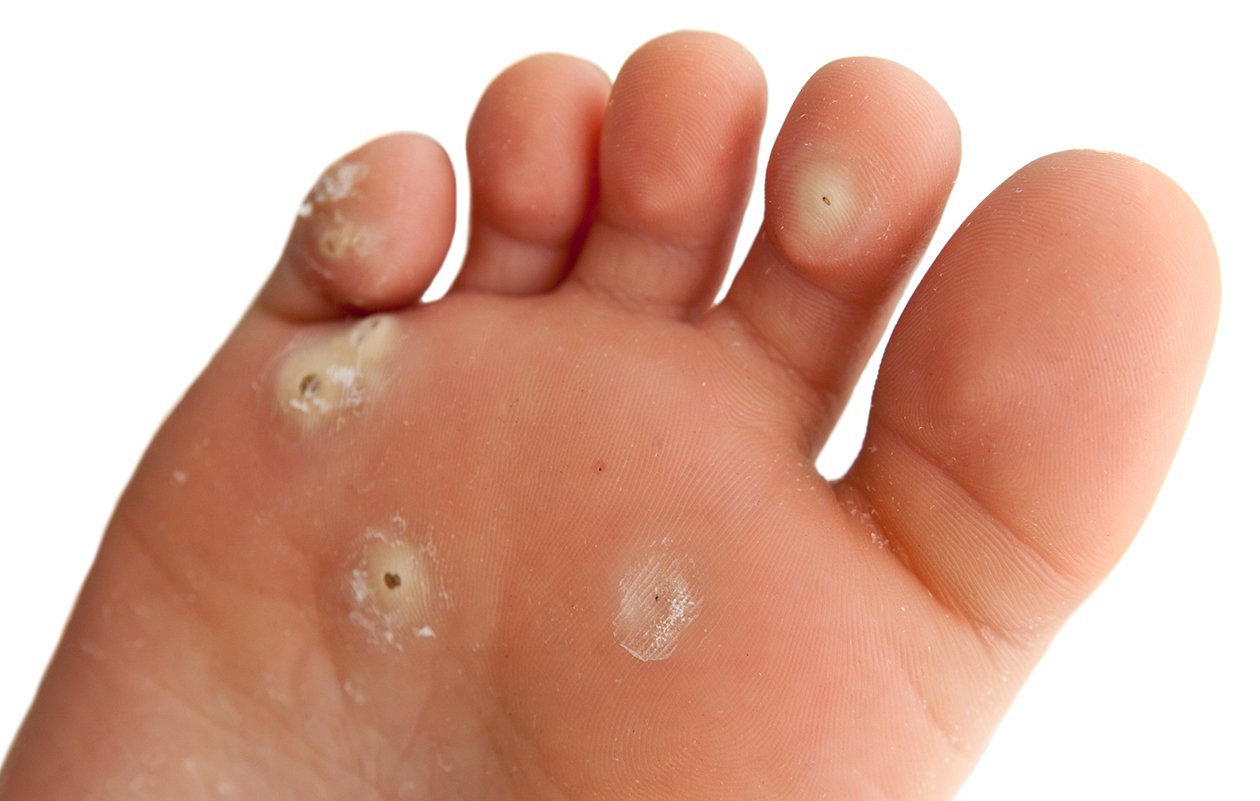
What Do They Look Like?
Verrucas can take on various appearances, but they often present as small, rough, and grainy growths with tiny black dots in the center. These black dots are often mistaken for “wart seeds,” but they are, in fact, small blood vessels supplying the verruca with nutrients. Verrucas may also have a thickened, calloused border, which distinguishes them from regular skin.
How Do Verrucas Spread?
Verrucas are highly contagious, and their spread can occur through direct or indirect contact. Here’s how it typically happens:
- Direct Contact: This occurs when the verruca-infected skin comes into direct contact with another person’s skin, potentially through activities like walking barefoot or sharing towels.
- Indirect Contact: Verrucas can also spread indirectly through contact with contaminated surfaces or objects, such as floors in communal areas. When a person walks on a surface infected with the virus and then steps onto a clean surface, they may unknowingly transfer the virus.
- Autoinoculation: Autoinoculation is a process where a person may inadvertently spread the virus to different areas of their body. This can occur when someone touches their verruca and then touches another part of their body, creating new verrucas in that area.
- Shared Footwear and Socks: If multiple individuals share shoes, socks, or other personal items that come into contact with the feet, the virus can be passed from one person to another through these items.
- Moist Environments: Verrucas are more likely to spread in warm, moist environments, such as swimming pools and public showers, where the virus can thrive. The virus can survive in such environments and infect individuals who walk barefoot in these areas.
- Weakened Immune System: Individuals with weakened immune systems are more susceptible to developing verrucas and may also be at a higher risk of spreading the virus to others.
- Scratching or Picking: Scratching or picking at a verruca can release the virus and potentially lead to the spread of the virus to other areas of the same person’s skin or to other individuals if there’s contact with the infected skin.
Who Treats Verrucas?
Now, let’s address a critical question – who treats verrucas? When it comes to these stubborn growths, a podiatrist is your go-to specialist. Podiatrists are trained to diagnose and treat a wide range of foot and ankle conditions, including verrucas.
Verruca Treatment: How Podiatrists Help
Verruca Treatment: How Podiatrists Help
A podiatrist is your trusted ally when it comes to addressing verrucas. These professionals are equipped with a range of tools and techniques to provide professional and effective treatment.
Let’s explore some of the key methods podiatrists use to help you get rid of verrucas:
- SWIFT Microwave Therapy: One of the most cutting-edge and popular treatments for verrucas is SWIFT microwave therapy. This non-invasive procedure employs microwave energy to target and eliminate verruca tissue. The high-frequency energy penetrates the skin, breaking down the infected cells and stimulating the body’s immune response. SWIFT therapy is known for its high success rate and minimal discomfort during the procedure. It’s an excellent option for those seeking a swift and efficient solution to their verrucas.
- Cryotherapy: Cryotherapy is another effective treatment for verrucas. It involves freezing the verruca with liquid nitrogen. The extreme cold destroys the affected tissue, allowing for the healthy skin to regenerate. Cryotherapy is a widely used method and is often employed when other treatments haven’t provided the desired results.
- Salicylic Acid Preparations: Podiatrists may recommend the use of salicylic acid preparations as part of a treatment plan. These topical solutions contain salicylic acid, which gradually softens and dissolves the verruca. This approach is more commonly used for less severe verrucas or in combination with other treatments.
- Debridement: Debridement is a procedure that involves the careful removal of the verruca. Podiatrists use specialized instruments, such as a scalpel, to reduce the thickness of the verruca and alleviate pressure and discomfort. Debridement is particularly useful when the verruca has become painful or is resistant to other treatments.
- Assessment and Prevention: Beyond the direct treatment of the verruca, podiatrists take a holistic approach to address any contributing factors. They assess your foot structure, footwear choices, and foot hygiene practices. By identifying and addressing these factors, podiatrists aim to prevent the recurrence of verrucas, ensuring that you don’t have to deal with these pesky growths in the future.
How to Prevent Verrucas and Their Spread
Preventing verrucas and their spread is just as important as treating them. Whether you’ve had verrucas in the past or you want to avoid the discomfort and inconvenience they bring, here are some key steps to help you maintain healthy and verruca-free feet:
- Foot Hygiene: Keep your feet clean and dry. Wash them regularly with mild soap and water, ensuring you dry them thoroughly, especially between the toes. Moisture can weaken the skin and make it more susceptible to verruca development.
- Protective Footwear: Choose your footwear wisely. Opt for shoes that provide proper support and cushioning. Avoid tight, ill-fitting shoes, especially those that put excessive pressure on specific areas of your feet.
- Avoid Barefoot Walking: Avoid walking barefoot in communal areas, such as swimming pools, locker rooms, and public showers. Verrucas are highly contagious and can spread through direct contact with contaminated surfaces.
- Change Socks and Shoes: Change your socks and shoes regularly, especially if your feet tend to sweat. Moist environments are favorable for verruca development. Rotating your footwear can help keep your feet dry and less susceptible to the virus.
- Foot Protection: Use waterproof footwear or verruca socks if you must walk in public showers or pool areas. These provide a protective barrier between your feet and potentially contaminated surfaces.
- Avoid Touching Verrucas: If you have a verruca, avoid touching or scratching it. Touching the verruca can release the virus, potentially leading to the development of new verrucas on your own skin or spreading the virus to others.
- Avoid Sharing Personal Items: Refrain from sharing towels, socks, or shoes with others, especially if you have a verruca. Sharing personal items can lead to the transmission of the virus.
Best Way to Get Rid of Verrucas Fast
You’ve just learned about verrucas, their causes, and the various treatments available. Now, let’s explore the best way to get rid of verrucas fast, and that’s by seeking professional treatment from a podiatrist.
Here’s why professional care is your best route to getting rid of verrucas SWIFTtly:
- Accurate Diagnosis: A podiatrist is skilled in identifying the type and severity of your verruca. They can differentiate between verrucas and other skin conditions, ensuring you receive the most appropriate treatment.
- Tailored Treatment Plans: Podiatrists create personalized treatment plans based on your unique situation. This tailored approach is crucial because not all verrucas are the same. What works for one person may not work for another. Professional care addresses your specific needs.
- Effective Treatment Methods: Podiatrists have a wide range of effective treatment methods at their disposal, including cutting-edge techniques like SWIFT microwave therapy, cryotherapy, and debridement. These methods have a track record of success, offering quicker relief.
- Minimizing Recurrence: While over-the-counter treatments may provide temporary relief, they often fall short in preventing verrucas from coming back. Podiatrists not only treat the verruca but also assess contributing factors like footwear and hygiene practices. This comprehensive approach reduces the risk of recurrence.
- Reduced Discomfort: Verrucas can be painful and uncomfortable, impacting your daily life. Seeking professional care can help alleviate this discomfort faster than trying to manage it with over-the-counter remedies.
- Expert Guidance: A podiatrist offers expert guidance on how to care for your feet during and after treatment. This includes advice on choosing the right footwear, maintaining proper foot hygiene, and taking steps to protect your feet from future verrucas.
By choosing professional treatment, you’re not just looking for a quick fix; you’re investing in the long-term health and comfort of your feet. Podiatrists understand the nuances of verruca treatment and are equipped with the knowledge and tools to provide efficient and lasting relief.
Conclusion
Now you know everything you need to know about verrucas, including how they spread and who treats them. By far the best way to get rid of verrucas fast is by visiting a podiatrist.
At Bucksfoot Clinic, we’re equipped with the latest technologies like SWIFT microwave therapy to ensure efficient and comfortable treatment. If you’re dealing with verrucas, don’t hesitate to reach out to us. We’re here to help you put your best foot forward!
Book an appointment today.
FAQs
Do podiatrists treat verrucas?
Yes, podiatrists are specialized healthcare professionals who diagnose and treat various foot and ankle conditions, including verrucas. They have the expertise to provide professional care and employ a range of treatments to effectively address verrucas and minimize discomfort.
Can you pick a verruca out with tweezers?
It is not advisable to attempt to pick a verruca out with tweezers or any other instruments on your own. Doing so can lead to infection, increased pain, and the risk of spreading the virus to other areas of your skin. It’s best to seek professional treatment from a podiatrist, who can safely and effectively address the verruca.
Why are verrucas so painful?
Verrucas can be painful due to the pressure they exert on the surrounding nerves and tissues. When you walk or stand, the pressure on the verruca can cause discomfort. Additionally, the virus can stimulate the body’s immune response, leading to inflammation and pain.
Do verrucas leave a hole?
Verrucas can sometimes leave a depression or small hole in the skin after they resolve or are treated. This is usually temporary and should gradually improve as the skin heals. It’s important to have a professional, such as a podiatrist, address verrucas to minimize scarring and lasting skin changes.
What is the best verruca treatment for stubborn verrucas?
For stubborn verrucas that have not responded to over-the-counter treatments, professional care from a podiatrist is often the most effective option. Cutting-edge treatments like SWIFT microwave therapy, cryotherapy, and debridement can be particularly successful in addressing stubborn verrucas. A podiatrist can assess the specific verruca and recommend the most suitable treatment for your case.
What does a dead verruca look like?
A dead verruca often appears flat or depressed, as it is no longer actively growing. The black dots or “wart seeds” (small blood vessels) in the verruca may disappear, and the surrounding skin might return to a more normal appearance. It’s important to consult a podiatrist for proper assessment and guidance during the treatment and post-treatment phases to ensure that the verruca is fully resolved.




Recent Comments