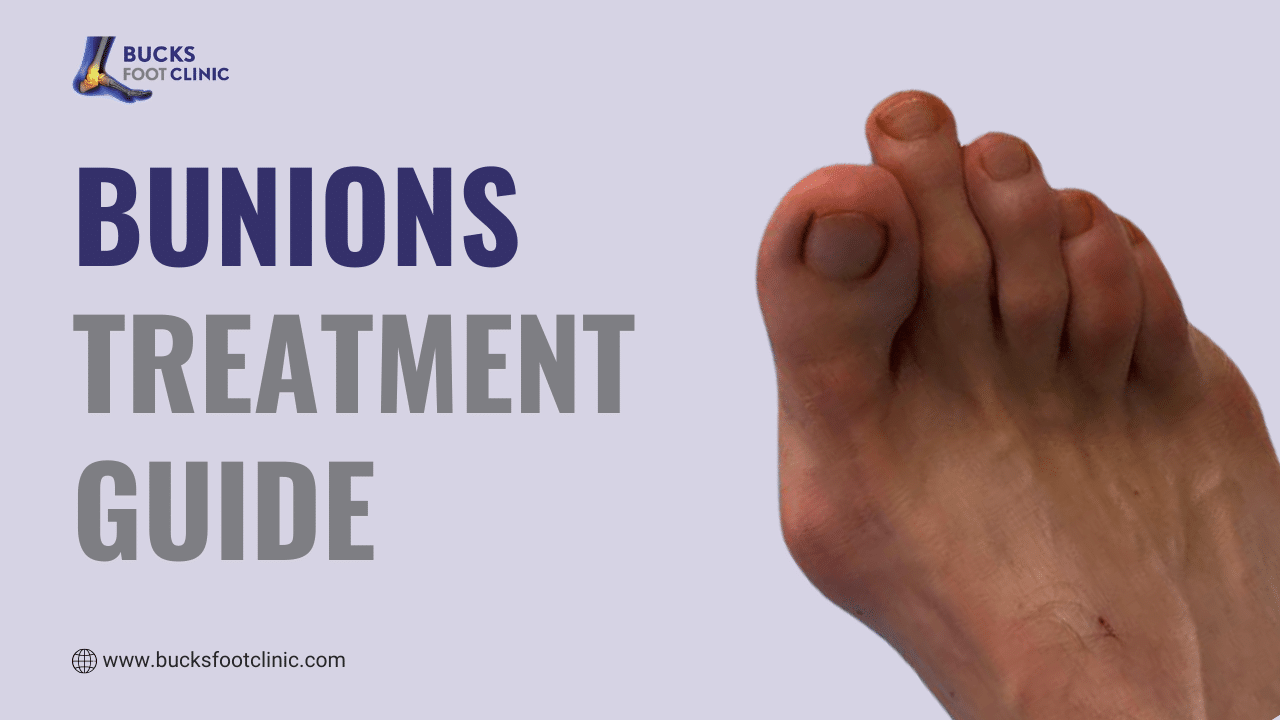
If you’ve noticed a bony bump forming at the base of your big toe, you’re not alone. Bunions (bunions treatment guide), medically known as hallux valgus, affect approximately 23% of adults in the UK, making them one of the most common foot deformities seen by podiatrists. This painful condition can significantly impact your daily life, from limiting your footwear choices to affecting your ability to walk comfortably.
Understanding bunions, their causes, and most importantly, your treatment options is crucial for maintaining healthy, pain-free feet. Whilst some people attempt home remedies, it’s essential to recognise the limitations of self-treatment and understand when professional podiatric care—or even surgery becomes necessary.
What Exactly Is a Bunion?
A bunion is far more than just a cosmetic inconvenience. It’s a progressive skeletal deformity where the first metatarsal bone shifts outwards whilst the big toe (hallux) angles inwards towards the second toe. This misalignment creates a prominent bony bump on the inside edge of your foot at the base of the big toe joint.
The medical term “hallux valgus” describes this deviation: “hallux” refers to the big toe, and “valgus” indicates the outward angulation. As the condition progresses, the joint becomes increasingly misaligned, and the fluid-filled sacs (bursae) around the big toe joint can become inflamed, causing swelling, redness, and severe pain.
The Progressive Nature of Bunions
What makes bunions particularly concerning is their progressive nature. Unlike a temporary injury that heals, bunions worsen over time without proper intervention. The deformity typically develops through several stages:
Mild bunions show a slight deviation of the big toe with minimal discomfort. The bump is small, and you may only experience occasional irritation when wearing tight shoes.
Moderate bunions present with noticeable deviation, regular pain, and difficulty finding comfortable footwear. The big toe may begin pushing against the second toe.
Severe bunions involve significant deformity where the big toe may overlap or underlap the second toe entirely. This stage often causes constant pain, difficulty walking, and can lead to additional foot problems such as hammertoes, corns, and calluses.
What Causes Bunions to Develop?
Understanding the root causes of bunions is the first step towards prevention and effective management. Research has identified several contributing factors:
1.Genetic Predisposition
Genetics plays the most significant role in bunion formation. If your parents or grandparents had bunions, you’re substantially more likely to develop them yourself. You inherit foot structure and bone shape, particularly the way your first metatarsal bone is positioned. Studies suggest that up to 70% of people with bunions have a family history of the condition.
2.Biomechanical Problems
Faulty foot mechanics significantly contribute to bunion development. Conditions such as overpronation (excessive inward rolling of the foot), flat feet, or flexible joints can disrupt the normal distribution of weight through the first metatarsal. This places abnormal stress on the big toe joint, eventually leading to bunion formation.
3.Ill-Fitting Footwear
Whilst tight shoes don’t directly cause bunions, they certainly accelerate their development and worsen symptoms. Shoes with narrow toe boxes, pointed toes, or high heels force the toes into unnatural positions, increasing pressure on the big toe joint. Women are disproportionately affected by bunions, partly due to the prevalence of constrictive footwear styles.
4.Inflammatory Conditions
Certain medical conditions, particularly rheumatoid arthritis and gout, can contribute to bunion formation through joint inflammation and damage. These conditions weaken the supportive structures around the joint, making deformity more likely.
5.Pregnancy and Hormonal Changes
Hormonal changes during pregnancy can loosen ligaments throughout the body, including those in the feet. Combined with weight gain and altered gait patterns, pregnancy can trigger bunion development or accelerate existing deformities.
6.Occupation and Lifestyle
Jobs requiring prolonged standing, particularly on hard surfaces, place continuous stress on the feet. Ballet dancers, athletes, and people whose occupations demand extended periods on their feet face increased risk.
How to Prevent Bunions: Your Essential Prevention Checklist
Prevention is always preferable to treatment. Whilst you cannot change your genetic predisposition, you can take proactive steps to reduce your risk or slow bunion progression:
Prevention Strategy #1: Choose Proper Footwear
- Select shoes with a wide, deep toe box that allows your toes to spread naturally
- Avoid pointed-toe shoes that squeeze toes together
- Limit high heels to special occasions; keep heels below 5 centimetres (2 inches) for daily wear
- Ensure shoes fit properly with adequate length and width
- Replace worn-out shoes that no longer provide proper support
Prevention Strategy #2: Maintain Healthy Foot Mechanics
- Have your gait and foot structure professionally assessed by a podiatrist
- Use custom orthotics if recommended to correct biomechanical issues
- Strengthen foot muscles through targeted exercises
- Address overpronation or flat feet early
Prevention Strategy #3: Manage Your Weight
- Maintain a healthy body weight to reduce stress on foot joints
- Each extra pound adds approximately four pounds of pressure on your feet
- Consult with healthcare professionals about safe weight management strategies
Prevention Strategy #4: Regular Foot Care and Monitoring
- Examine your feet regularly for early signs of bunion development
- Measure both feet when buying shoes, as foot size can change over time
- Schedule annual podiatric assessments, especially if you have risk factors
- Address foot pain promptly rather than ignoring it
Prevention Strategy #5: Lifestyle Modifications
- Take regular breaks if your job requires prolonged standing
- Use anti-fatigue mats when standing for extended periods
- Vary your footwear throughout the week
- Incorporate foot stretches and exercises into your daily routine
Prevention Strategy #6: Early Intervention
- Seek professional advice at the first sign of bunion development
- Don’t wait until pain becomes unbearable
- Early conservative treatment can significantly slow progression
Home Remedies for Bunions: Understanding the Limitations
Many people attempt to manage bunions at home, and whilst some remedies can provide temporary relief, it’s crucial to understand their significant limitations.
Ice Therapy
What it does: Applying ice packs to the bunion can reduce inflammation and provide temporary pain relief.
Limitations: Ice only addresses symptoms, not the underlying structural deformity. It cannot reverse or slow bunion progression. Relief is temporary, typically lasting only a few hours. Overuse can cause skin damage or frostbite.
Over-the-Counter Pain Relief
What it does: Non-steroidal anti-inflammatory drugs (NSAIDs) like ibuprofen can reduce pain and swelling.
Limitations: Medication masks symptoms without addressing the cause. Long-term use carries risks including stomach ulcers, cardiovascular problems, and kidney damage. Pain relief is temporary and stops when you discontinue the medication. NSAIDs cannot prevent bunion progression.
Bunion Pads and Cushions
What they do: Gel pads or moleskin cushions reduce friction between the bunion and your shoe.
Limitations: These provide only symptomatic relief and don’t correct the deformity. They can make shoes feel tighter, potentially worsening the problem. The bunion continues to progress underneath the padding. They’re merely a temporary comfort measure.
Toe Spacers and Separators
What they do: Silicone or foam devices placed between toes attempt to realign the big toe.
Limitations: Research shows minimal effectiveness for established bunions. They cannot overcome the forces of weight-bearing and walking. Most people find them uncomfortable to wear for extended periods. They may provide temporary relief but don’t address skeletal misalignment. Once removed, the toe returns to its deviated position.
Bunion Splints and Braces
What they do: Rigid or semi-rigid devices worn at night attempt to straighten the big toe.
Limitations: Scientific evidence for their effectiveness is extremely limited. They cannot reverse established skeletal deformity. The forces applied are insufficient to overcome the structural changes. Any perceived improvement is typically temporary. They can be uncomfortable and disrupt sleep.
Toe Exercises and Stretches
What they do: Exercises aim to strengthen foot muscles and improve flexibility.
Limitations: Whilst beneficial for overall foot health, exercises cannot correct bone misalignment. They may provide minor symptom relief but won’t reverse bunions. Results are modest at best. They must be performed consistently indefinitely.
Warm Foot Soaks
What they do: Soaking feet in warm water can soothe aching feet and relax muscles.
Limitations: Purely symptomatic relief with no effect on the bunion itself. Benefits last only while soaking and shortly afterwards. Does nothing to address structural problems.
The Fundamental Problem with Home Remedies
Here’s the crucial truth: bunions are a skeletal deformity. No amount of padding, splinting, exercising, or soaking can realign bones that have shifted out of position. Home remedies can only manage symptoms temporarily—they cannot and will not:
- Correct the bone misalignment
- Stop or reverse bunion progression
- Address biomechanical causes
- Prevent secondary complications
- Provide permanent pain relief
This is why professional podiatric assessment and treatment are essential for anyone with bunions.
Why a Podiatrist Is Better Than Home Remedies
Whilst home remedies might offer temporary comfort, they fundamentally cannot address the structural and biomechanical issues underlying bunions. Here’s why professional podiatric care is superior and often essential:
Accurate Diagnosis and Assessment
Podiatrists possess specialised training to accurately diagnose bunions and differentiate them from other conditions such as gout, arthritis, or stress fractures. They can assess the severity of your bunion, identify contributing biomechanical factors, and develop a comprehensive treatment plan tailored to your specific situation.
At Bucks Foot Clinic, our experienced podiatrists conduct thorough examinations including gait analysis, joint mobility testing, and assessment of your foot structure. We may recommend imaging such as X-rays to evaluate the degree of bone misalignment and identify any arthritic changes.
Addressing Root Causes, Not Just Symptoms
Unlike home remedies that merely mask pain, podiatrists identify and address the underlying causes of your bunion. This might include overpronation, flat feet, or other biomechanical abnormalities that home treatment cannot detect or correct.
Custom Orthotics and Professional Devices
Podiatrists can provide custom-made orthotic devices specifically designed for your foot structure. These medical-grade orthotics differ vastly from over-the-counter insoles:
- They’re precisely crafted based on moulds or scans of your feet
- They correct specific biomechanical problems
- They redistribute pressure away from the bunion
- They can significantly slow bunion progression
- They improve overall foot function and comfort
Research demonstrates that properly fitted custom orthotics provide substantial symptom relief and can slow bunion progression in many patients.
Professional Padding and Strapping Techniques
Podiatrists employ advanced padding and strapping techniques that far exceed what you can achieve at home. These professional applications:
- Use medical-grade materials
- Are precisely positioned for maximum benefit
- Can be adjusted based on your response
- Provide superior comfort and protection
Comprehensive Treatment Plans
Professional bunion management involves multiple strategies working together:
- Footwear recommendations specific to your foot shape and bunion severity
- Gait retraining to reduce stress on the affected joint
- Strengthening and flexibility exercises properly taught and monitored
- Inflammation management through various therapeutic modalities
- Regular monitoring to track progression and adjust treatment
Early Intervention Advantages
Seeing a podiatrist early in bunion development offers significant advantages. Early professional intervention can:
- Substantially slow or even halt progression
- Prevent secondary complications like hammertoes
- Maintain better joint function
- Reduce pain more effectively
- Potentially avoid or delay the need for surgery
Expert Guidance on Surgical Options
When conservative treatment proves insufficient, podiatrists provide expert guidance on surgical options. They can explain different surgical techniques, help you understand the risks and benefits, refer you to appropriate orthopaedic surgeons, and manage your post-operative care.
If you’re experiencing bunion pain or have noticed a bump forming on your big toe, don’t wait for the problem to worsen. Contact Bucks Foot Clinic today on 01494 434366 to schedule a comprehensive foot assessment. Early professional intervention can make a significant difference in your outcome.
How to Fix Bunions: Comprehensive Treatment Options
Treatment approaches vary depending on bunion severity, pain levels, and how much the condition impacts your daily life. Here’s a detailed breakdown of available options:
Conservative (Non-Surgical) Treatments
Footwear Modifications The cornerstone of conservative bunion management involves proper footwear. Your podiatrist will recommend shoes with:
- Wide, deep toe boxes allowing natural toe spread
- Soft, flexible uppers that don’t press on the bunion
- Good arch support
- Low heels (under 5 centimetres)
- Adequate length to prevent toe crowding
Custom Orthotic Therapy Medical-grade custom orthotics prescribed by your podiatrist can:
- Correct overpronation and other biomechanical faults
- Redistribute pressure across your foot
- Support your arches properly
- Reduce stress on the big toe joint
- Slow bunion progression significantly
Padding and Protective Devices Professional-grade bunion pads, sleeves, and separators positioned by your podiatrist provide superior protection compared to over-the-counter products. These are custom-fitted to your specific bunion and footwear.
Physical Therapy and Exercises Supervised exercise programmes can improve foot strength, flexibility, and function. Your podiatrist may recommend specific exercises or refer you to a physiotherapist specialising in foot conditions.
Anti-Inflammatory Treatments Beyond oral medications, podiatrists can provide:
- Cortisone injections to reduce severe inflammation
- Topical anti-inflammatory preparations
- Cold therapy protocols
- Advice on managing inflammatory flares
Activity Modification Your podiatrist will guide you on:
- Which activities to avoid or modify
- Alternative exercises that don’t stress the bunion
- Proper foot positioning during activities
- Rest and activity balance
Surgical Treatment Options
When conservative treatment fails to provide adequate relief, or when the bunion severely impacts your quality of life, surgery becomes the appropriate option. There are over 100 different surgical techniques for bunion correction, but they generally fall into these categories:
Osteotomy Procedures The most common surgical approach involves cutting and realigning the metatarsal bone. Different osteotomy techniques include:
- Chevron Osteotomy: Suitable for mild to moderate bunions, this V-shaped cut in the metatarsal head allows the bone to be shifted and secured with screws.
- Scarf Osteotomy: Ideal for moderate to severe bunions, this Z-shaped cut provides excellent stability and correction.
- Proximal Osteotomy: Used for severe bunions, this procedure addresses the bone closer to the ankle where the deformity originates.
Arthrodesis (Fusion) For severe bunions with significant arthritis, surgeons may fuse the big toe joint. Whilst this limits joint motion, it provides pain relief and excellent correction for severe deformities.
Arthroplasty (Joint Resurfacing) In selected cases, particularly in older patients, part of the joint may be removed or resurfaced to relieve pain and correct deformity.
Soft Tissue Procedures These may be combined with bone procedures and involve:
- Releasing tight ligaments on one side of the joint
- Tightening loose ligaments on the opposite side
- Repositioning tendons
Recovery and Outcomes
Surgical outcomes vary depending on the procedure, but most patients experience:
- Significant pain reduction
- Improved foot function
- Better footwear options
- Enhanced quality of life
Recovery typically requires:
- 6-8 weeks of limited weight-bearing or special footwear
- 3-6 months for return to normal activities
- Up to 12 months for complete healing and final results
Success rates for bunion surgery are generally high, with 85-90% of patients satisfied with their outcomes. However, recurrence is possible, particularly if underlying biomechanical problems aren’t addressed or if genetic factors are strong.
When to See a Podiatrist vs When to See a Surgeon
Understanding when to seek different levels of professional care is crucial for optimal bunion management.
See a Podiatrist When:
You first notice bunion development – Early assessment allows for preventive strategies that can significantly alter the course of your condition. Don’t adopt a “wait and see” approach.
You experience any foot pain – Even mild discomfort warrants professional evaluation. Pain indicates that problematic forces are at work in your foot.
Your bunion limits footwear choices – If you’re struggling to find comfortable shoes, a podiatrist can help with footwear recommendations and may provide solutions that make more shoes wearable.
You have risk factors – If bunions run in your family, you have flat feet, or you’ve been diagnosed with inflammatory arthritis, regular podiatric monitoring is wise.
Home remedies aren’t working – If you’ve tried over-the-counter treatments without success, it’s time for professional intervention.
You want to prevent progression – Proactive patients who seek care early often achieve the best long-term outcomes.
You have related conditions – Conditions like diabetes, peripheral arterial disease, or arthritis require specialised podiatric oversight of any foot problems.
The bunion is changing – Rapid progression or sudden changes in appearance or pain warrant prompt assessment.
You’re developing secondary problems – If corns, calluses, hammertoes, or other issues are developing alongside your bunion, comprehensive professional care is needed.
Your bunion is affecting your activity level – If you’re avoiding activities you enjoy due to bunion pain, don’t accept this diminished quality of life.
Podiatrists Should Refer You to a Surgeon When:
Conservative treatment has failed – If you’ve undergone appropriate conservative treatment for 3-6 months without adequate improvement, surgical consultation becomes appropriate.
Pain is severe and persistent – Unrelenting pain that significantly impacts daily life despite conservative measures indicates surgery may be necessary.
The deformity is progressing rapidly – Fast progression despite treatment suggests conservative measures won’t be sufficient.
Secondary complications have developed – When bunions cause hammertoes, chronic bursitis, or other complications that don’t respond to conservative care.
Joint damage is evident – X-rays showing significant arthritis in the big toe joint may indicate surgery is the best option.
The bunion severely limits function – If you cannot walk comfortably, cannot wear any reasonable shoes, or cannot perform necessary activities, surgery should be considered.
You have realistic expectations – Good surgical candidates understand the recovery process, have appropriate expectations, and are committed to post-operative protocols.
Your general health permits surgery – You must be healthy enough to undergo surgery and recover appropriately.
Red Flags Requiring Urgent Assessment:
Certain situations demand immediate professional evaluation:
- Signs of infection (increased redness, warmth, pus, fever)
- Sudden severe pain
- Inability to bear weight
- Skin breakdown or ulceration over the bunion
- Numbness or tingling in the toes
- Sudden colour changes in the foot
If you experience any of these symptoms, contact Bucks Foot Clinic immediately on 01494 434366.
The Bucks Foot Clinic Approach to Bunion Care
At Bucks Foot Clinic, we understand that every bunion is unique, and every patient has different needs, lifestyles, and goals. Our comprehensive approach includes:
Thorough Initial Assessment We take time to understand your complete medical history, examine your feet and gait thoroughly, and identify all contributing factors to your bunion development.
Personalised Treatment Plans We don’t believe in one-size-fits-all solutions. Your treatment plan reflects your specific condition, lifestyle, activity level, and goals.
Conservative Treatment Excellence We exhaust appropriate conservative options before considering surgical referral, utilising the latest evidence-based treatments including custom orthotics, advanced padding techniques, and comprehensive footwear guidance.
Surgical Guidance When Needed If surgery becomes necessary, we provide honest, expert guidance on your options and work closely with excellent orthopaedic foot and ankle surgeons in the Buckinghamshire area.
Ongoing Support and Monitoring Bunion management is often a long-term partnership. We provide regular follow-ups to monitor your condition and adjust treatment as needed.
Patient Education We believe informed patients achieve better outcomes. We take time to explain your condition, treatment options, and preventive strategies in clear, understandable terms.
Take the First Step Towards Healthier Feet
Bunions don’t improve on their own, and delaying professional care typically leads to worse outcomes, more limited treatment options, and potentially more complex surgery if it becomes necessary. Early professional intervention offers the best chance of managing your bunion effectively and maintaining an active, pain-free lifestyle.
Whether you’ve just noticed a small bump forming, you’re experiencing increasing pain, or you’re frustrated with ineffective home remedies, the team at Bucks Foot Clinic is here to help.
FAQ’s
Q: What is a bunion?
A: A bunion is a deformity where the big toe moves toward the second toe and a bony bump forms at the base of the big toe joint.
Q: What causes bunions?
A: Bunions are mainly caused by genetics and foot structure, but poor footwear, biomechanical issues, and certain health conditions can contribute.
Q: What are the common symptoms of bunions?
A: Pain, swelling, redness, a visible bump on the big toe joint, and difficulty wearing shoes.
Q: Can bunions be fixed at home?
A: No. Home treatments may relieve pain but cannot correct the bone alignment.
Q: How are bunions treated without surgery?
A: Treatment may include proper footwear, custom orthotics, padding, exercises, and reducing pressure on the joint.
Q: Do shoes make a difference for bunions?
A: Yes. Shoes with a wide toe box and good support can reduce pain and irritation.
Q: Can orthotics help bunions?
A: Yes. Orthotics help improve foot alignment and reduce stress on the joint.
Q: When is bunion surgery needed?
A: Surgery may be considered if pain is severe, long-lasting, or affects daily activities.
Q: When should I see a podiatrist?
A: If you notice a bunion forming, have pain, or struggle with footwear.
Don’t let bunion pain control your life. Contact Bucks Foot Clinic today on 01494 434366 to schedule your comprehensive bunion assessment. Our experienced podiatrists will develop a personalised treatment plan to get you back to the activities you love.
Your feet carry you through life they deserve expert professional care. Take that important first step towards healthier, happier feet by calling us today.
Bucks Foot Clinic: Your trusted partner in foot health, serving the Buckinghamshire community with expert, compassionate podiatric care.

Recent Comments